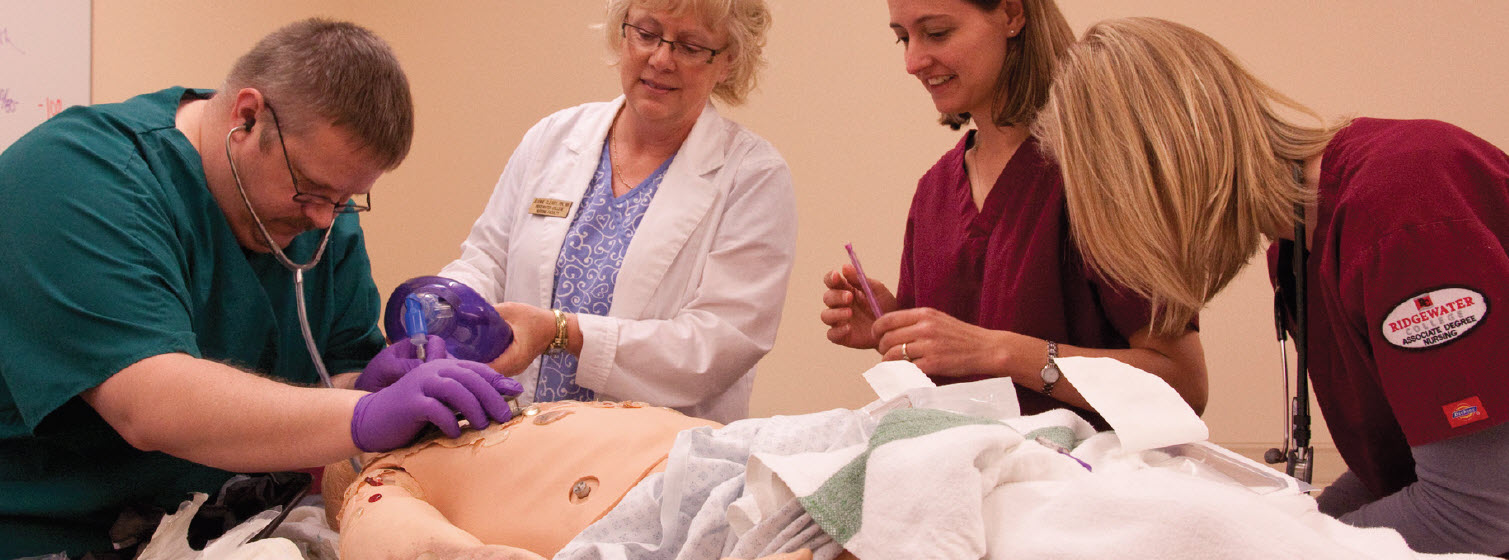
A growing body of evidence shows that clinical skills acquired via simulation transfer directly to improved patient care and better outcomes. When paired with deliberate practice, simulation-based education is found to be superior to traditional clinical education for a wide range of skills acquisition.2
One such study indicates that simulation promotes engagement in several ways:
- Flow:
Students were absorbed in the task at hand.
- 兴趣:
学生表现出兴趣,这是享受,积极的讨论和幽默所证明的。
- 关联:
就情境临床实践,考试准备和获得有关临床决策的反馈而言,模拟与仿真相关。3

