
Pocus的精通可以分为三个领域:
- Image acquisition:
Knowing when and where to scan - Image interpretation:
生成图像并知道何时足以解释和数据提取 - Integration into clinical care:
Making decisions based on complete data (history, physical and POCUS images)11
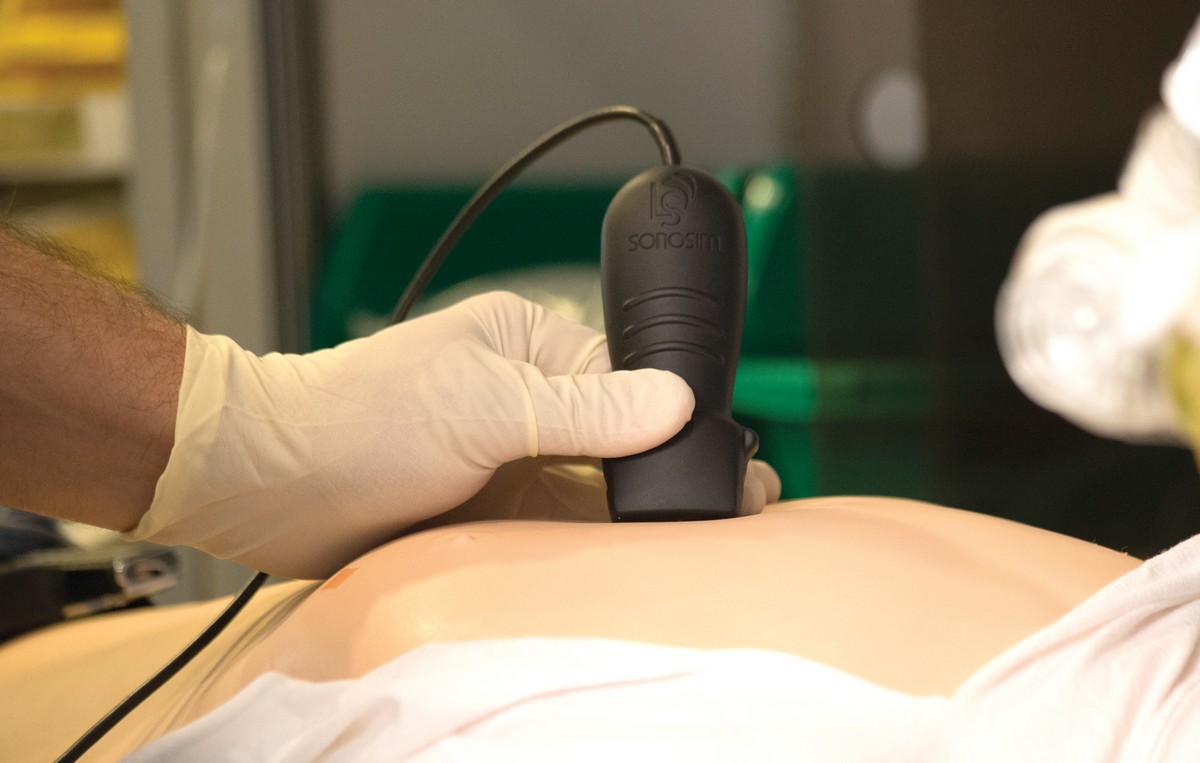

超声波不仅仅用于孕产妇保健practices. Having come a long way since its roots in military and industrial settings, today ultrasound is well-established as a crucial technology across a range of diagnostic and therapeutic applications. The uses vary from determining the size and sex of a fetus to boosting the accuracy of a needle biopsy to treating a soft-tissue injury. Further, bedside point-of-care ultrasound (POCUS) has evolved into a valuable addition to an acute care clinician’s toolbox in settings such as emergency and intensive care medicine. It’s fast, improves diagnostic accuracy and informs treatment plans by condensing the list of viable diagnostic etiologies.1
Herein, we discuss the applications of point-of-care ultrasound as well as why you might want to consider integrating it into your existing simulations.
Pocus发现充当诊断难题的一大部分,通常表明了护理途径的下一步。
POCUS can help reinforce core anatomy and physiology concepts, illustrate pathology and disease processes, and facilitate mastery of the physical examination. For these reasons, organizations ranging from the American Academy of Emergency Medicine to the American Institute for Ultrasound in Medicine, have advocated for POCUS as an important element of undergraduate medical education.2 3
However, there are two caveats. First, POCUS is operator dependent. Confidence and competence in image acquisition and interpretation are essential, as is the ability to incorporate one’s findings into clinical decision-making.4Developing the necessary operator competence in ultrasound often proves problematic, as it currently consists of a “see one, do one” approach that requires patients, standardized patients, commercial training models or cadavers — all at substantial cost.
Second, today’s ultrasound training typically lacks an emphasis on critical thinking and decision-making components — vital in emergency and intensive care settings.

As point-of-care ultrasound becomes an increasingly prevalent imaging modality, medical schools and residency programs are beginning to incorporate more robust ultrasound training into the curricula. Experts can’t help but draw a parallel to the history of anesthesia educators, who turned to simulation in order to train basic skills in a realistic context.
Until the 1990s, anesthesiology residents faced challenges in achieving clinical competency while maintaining patient safety. Many of the technical and non-technical skills required for anesthesia practice — from difficult airway management and lung separation to effective teamwork — are ideally acquired by exercises and experiences rather than traditional lectures.
The emergence of high-fidelity mannequin simulators and simulation-based training effectively addressed these challenges. Anesthesiology residents trained with simulators were found to respond more quickly, perform better and deviate less from accepted procedures.5Other researchers reported better cardiopulmonary resuscitation performance6,降低与中央导管插入有关的成本和并发症7, higher scores in cardiopulmonary bypass weaning and superior non-technical skills in simulation training groups.
为什么医疗模拟培训如此有效?经验表明模拟…
• Serves as an alternative to a live patient.
•是基于体验的学习。
•提供不同水平的忠诚度。
• Increases engagement and maximizes retention.
• Allows for debriefing.
•改善团队合作。
Simulation training is particularly well-suited for mastering point-of-care ultrasound, which is a required core competency for emergency medicine and other specialties. It is rapid, accurate, repeatable, cost-effective, noninvasive and without the risk of radiation, and may be used in both stable and unstable patients. It may also be performed parallel to physical examination, resuscitation and stabilization, which can add significant value to medical schools and residency programs’ ultrasound training.9

对于诊断和治疗工具,例如超声波,模拟是寻求改善患者安全的关键组成部分,因为它:12
美国医学院协会的一项调查发现,超过80%的医学院在课程的所有四年内都纳入了基于模拟的教学。10Among nursing schools, 87% have incorporated simulation-based training with high- or medium-fidelity mannequins within the curriculum.11
Many schools have access to simulation equipment — its use simply has yet to reach full capacity when it comes to ultrasound. That means the majority of today’s chief residents and clinical directors did not experience the value of simulation firsthand in their own ultrasound training, and may not recognize the opportunity it presents to optimize the teaching of this clinical skill.
随着Point Pare-Pare Ultrasound快速成为临床检查的扩展,基于模拟的教育是满足新兴教育需求的首选工具,并最终改善了患者的安全性和结果。
With team training solutions such as theLaerdal SonoSim Ultrasound Solutionnow available, programs that currently use Laerdal simulators may find they can be expanded to include POCUS training capabilities.
